“How can complex vascular malformations be treated more precisely today – and what does that mean in concrete terms for those affected?” Answers to this question were provided by the specialist event “BEST Practice: Bleomycin Electrosclerotherapy and Electroembolotherapy”, which took place on 27 September 2025 in the conference room of RoMed Klinikum Rosenheim. Organised by the Bundesverband Angeborene Gefässfehlbildungen e.V. in close cooperation with Prof. Dr. Natascha Platz Batista da Silva from the RoMed clinics, the event brought together specialist physicians, therapists, and patient representatives from across the German-speaking region.
As a patient representative of Association Angiodysplasia Switzerland – one of the German federal association’s partner organisations – I had the opportunity to attend this fascinating specialist event. The following report reflects my personal impressions and insights from a patient perspective.
The Bundesverband Angeborene Gefässfehlbildungen e.V.

The Bundesverband Angeborene Gefässfehlbildungen e.V. was founded in 2006 from three existing self-help groups and today has around 505 members. The association is funded through lump-sum support from statutory health insurance funds (GKV), project funding, support from Aktion Mensch, as well as donations and membership fees.
The association’s reach extends far beyond Germany: as part of a Europe-wide connected network, the federal association is linked with organisations such as DiGGefa, ACHSE e.V., EURORDIS, and VASCERN. Other partner organisations include Angiodysplasia Switzerland, Mutkoerperchen.at, HHT Germany – Morbus Osler Selbsthilfe, and Interessengemeinschaft Sturge-Weber-Syndrom e.V.

RoMed Clinics: Interdisciplinary Centre for Vascular Anomalies

Prof. Dr. Natascha Platz Batista da Silva presented the interdisciplinary centre for vascular anomalies at the RoMed clinics, which serves as a regional expertise hub for the diagnosis and treatment of congenital vascular malformations. In addition to individual treatment concepts, the centre also offers second opinions, consultations, and assessments, and is integrated into the reference network for rare vascular diseases.
Also worth mentioning is the multicentre case conference VasMut, which enables supraregional cooperation between specialised centres and discusses difficult cases in an interdisciplinary setting. For patients, who often have a long diagnostic journey behind them, such a structure is a real source of support.
Specialist lectures: From understanding to therapy
Typical symptoms and the patient journey
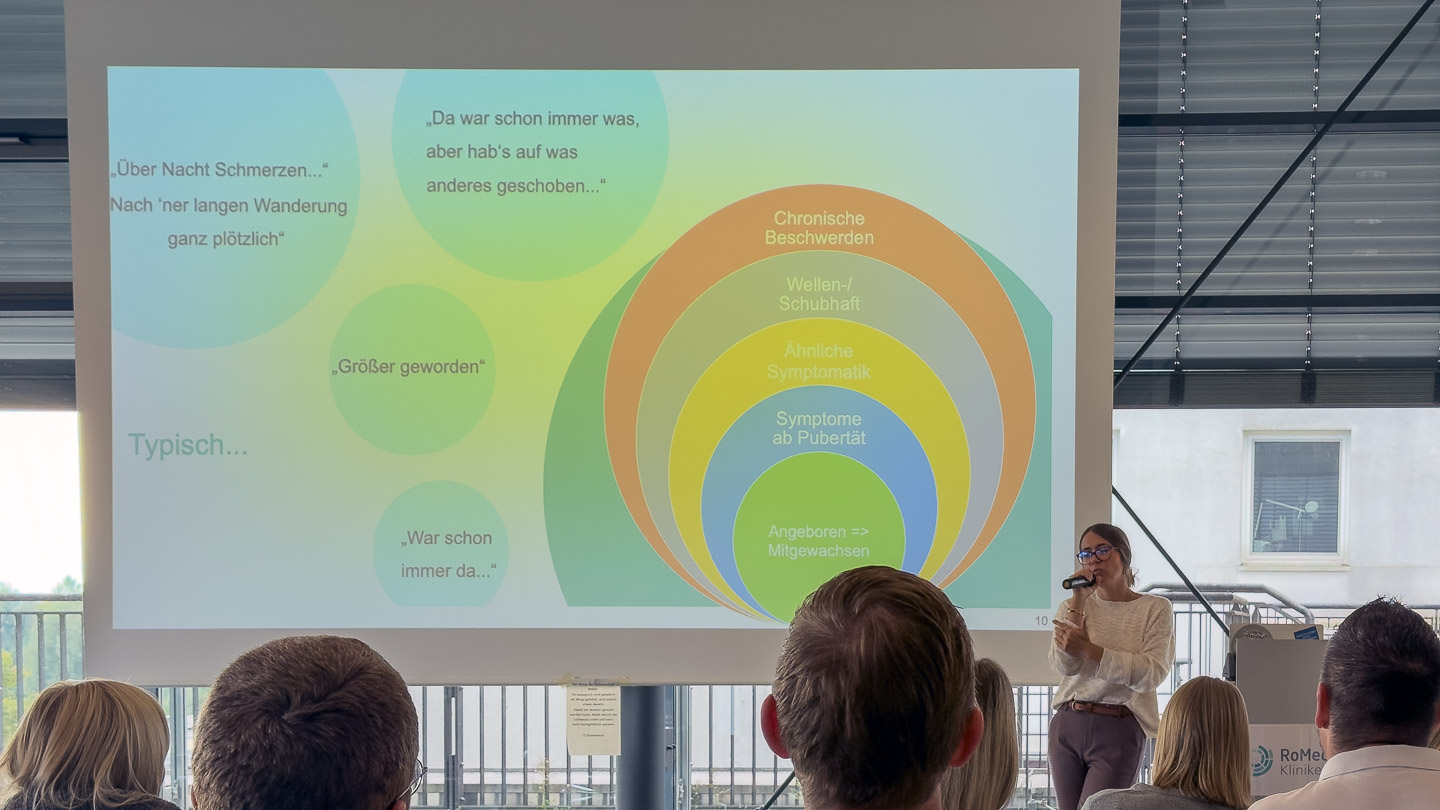
A particularly impressive lecture highlighted the typical symptom patterns of people with congenital vascular malformations. The presentation made clear how varied and often non-specific the symptoms are: many affected individuals have known about their malformation since birth, while others only notice it during puberty – often triggered by hormonal changes, infections, or trauma.
Typical descriptions from affected individuals such as “It was always there”, “It got bigger”, or “Pain overnight” illustrate the gradual development and the uncertainty that often lasts for years until the correct diagnosis is made. The message to the audience was clear: patients need reliable, medically well-founded points of contact.
Paradigm shift in the understanding of vascular anomalies

Another key topic was the scientific paradigm shift in the classification of vascular anomalies. Whereas in the past the main distinction was between vascular tumours and vascular malformations, the current ISSVA classification (International Society for the Study of Vascular Anomalies) establishes a much more differentiated system. This “Changing Minds” moment has direct implications for diagnosis and therapy selection – and thus for the lives of those affected.
Overview of therapy options
The lectures provided a comprehensive overview of the different treatment approaches depending on the type of malformation: venous malformations (VM) and lymphatic malformations (LM) are treated with conventional sclerotherapy – for example with bleomycin or alcohol-based substances such as Picibanil or Discogel. Arteriovenous malformations (AVMs) require embolisation using permanent liquid embolic agents, while capillary malformations (CM) are treated with laser therapy.
BEST and BEET – Electroporation for slow-flow and high-flow malformations
Basic principle: Electroporation with bleomycin

Prof. Platz Batista da Silva presented two related, yet clearly distinct procedures, both based on the principle of electroporation with bleomycin: weak electrical impulses temporarily permeabilise the cell membranes of the vessel walls, which significantly increases the uptake of the cytostatic agent bleomycin into the cells and enables targeted tissue destruction.
BEST (Bleomycin Electrosclerotherapy) is aimed at slow-flow malformations – namely venous malformations (VM) and lymphatic malformations (LM). The active substance is applied interstitially – meaning directly into the tissue between the cells – either as a continuous infusion or as an injection. This allows for a broader-area treatment than classical sclerotherapy procedures.
Who is BEST suitable for?
The indications for BEST include in particular:
- therapy-refractory lesions
- extensive findings
- oral and genital malformations
- malformations with increased volume
- microcystic lymphatic malformations
BEET – Bleomycin Electroembolotherapy for arteriovenous malformations (AVMs)
For high-flow malformations – especially arteriovenous malformations (AVMs) – Prof. Platz Batista da Silva used the term BEET (Bleomycin Electroembolotherapy). The crucial difference is this: in BEET, the AVM nidus is accessed directly via a catheter, from where the bleomycin is applied interstitially and infused over 10 minutes – meaning administered continuously.
A central clinical principle, which Prof. Platz Batista da Silva emphasised strongly, is this: the nidus must be completely eliminated. Incomplete treatment of the nidus – the actual core area of the AVM in which the pathological vascular connections between arteries and veins arise – leads with high probability to recurrence. Especially in AVMs, the radical completeness of treatment is therefore crucial for long-term therapeutic success.
The fact that BEET exists at all today is largely thanks to Prof. Wohlgemuth: he asked the question “If it works in slow flow, why not in high flow as well? Are we doing something wrong?” and thereby provided the decisive impetus to transfer the electroporation technique to high-flow malformations.
Clinical experience: BEST vs. Aethoxysklerol
Particularly impressive was the contribution of an affected patient who spoke as a presenter and reported from her own experience. She described how she experienced BEST in comparison with Aethoxysklerol: BEST offers a broader-area treatment option and, in her case, led to fewer recanalisations – that is, the reopening of previously treated vessels – as well as less long-term swelling. However, in her case postoperative pain during the first two days after BEST was stronger than after Aethoxysklerol, and haematomas as well as electrode puncture marks may occur, although these fade after a few weeks.
Practical workstation session

A central programme item in the afternoon was a hands-on workstation session in the angiography suite. Prof. Dr. Natascha Platz Batista da Silva demonstrated the technique live on a tissue model – clearly and interactively. For us as patients, this was a particularly impressive moment: a look behind the scenes into a world that usually remains hidden from us – and that can now help us better understand what actually happens during an intervention.
Patient perspective: My personal conclusion
As a patient representative, taking part in this event was deeply impressive for me. It is rare to experience, within a single event, such a dense combination of scientific knowledge, clinical experience reports, and practical demonstration.
I was impressed by the openness of the speakers in clearly addressing unresolved questions as well – for example regarding the further development of BEET or the question of how completely the nidus in AVMs needs to be eliminated.
But what impressed me most as a patient representative was this: Prof. Platz Batista da Silva and all the speakers found a language that makes these complex medical issues understandable for patients as well. That is by no means self-evident – and it is invaluable. Because only those who understand what is happening to them and what options exist can truly make decisions about their own therapy on an equal footing.